For Tillman Scholar and veteran Andrew Fisher, his time at medical school is not just spent learning; he’s also sharing his knowledge with fellow medical students. Not all medical students at Texas A&M are interested in emergency medicine or in military careers post-graduation, but a recent Tactical Combat Casualty Care course at Fort Hood is helping them learn how to identify and treat wounds in trauma situations if they should ever occur.
Fisher stands out among most of his medical school peers, and it isn’t just because he’s quite tall. As a physician assistant with the 75th Army Ranger Regiment, he participated in almost 600 combat missions and took care of more than 100 people at the point of injury.
“We are extremely proud to welcome veterans like Andrew Fisher into our college,” said Carrie L. Byington, MD, dean of the Texas A&M College of Medicine, senior vice president of Texas A&M University Health Science Center and vice chancellor for health services at The Texas A&M University System. “We’re an institution built on a close relationship to the military and we were created 40 years ago to improve the lives of veterans through medicine. Opportunities like this help diversify the clinical and research opportunities for all students.”
Fisher is experienced in leading medical training for his Ranger unit. Now he’s brought his emergency medicine knowledge with him and is helping his fellow classmates to learn some key skills that they can utilize wherever they may find themselves practicing medicine.
“I want as many medical students as possible to have real skills to be able to react and respond in any trauma situation,” Fisher said. “This is the same training we gave every Army Ranger on how to treat the three most prevalent causes of preventable death in combat: tension pneumothorax, airway obstruction, and massive bleeding from an extremity.”
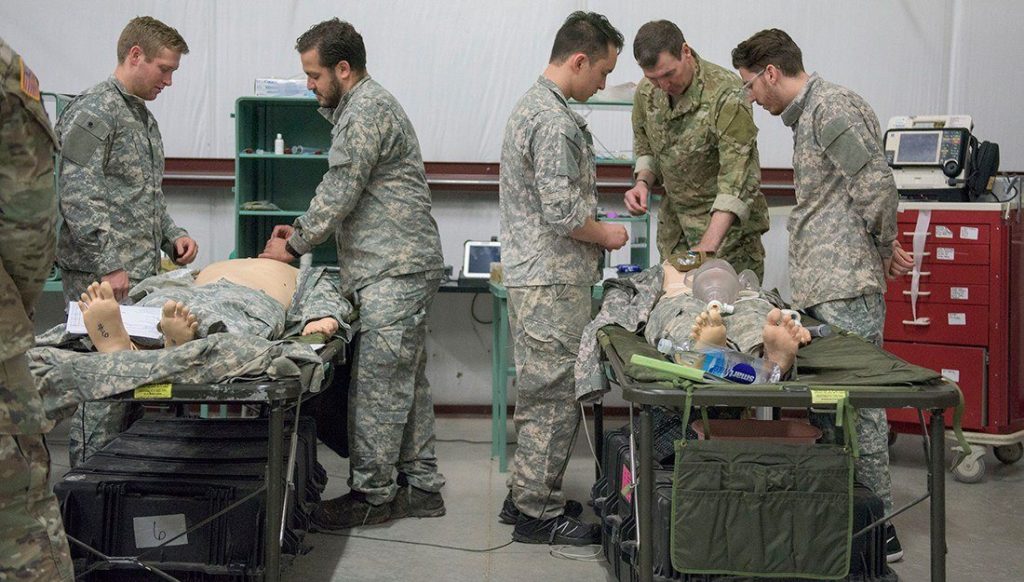
The course comes with a certification that lasts for two years and is accredited by the National Association of Emergency Medicine Technicians. In addition to lectures, the students also learn the same methods the Army uses to treat wounds in combat. During an all-day simulation on September 9th, the students practiced what they learned.
The simulation, which was meant to mimic the hectic situation encountered on a battlefield, included the sound of gunfire, smoke and many other things that make treatment in the field difficult.
Mannequins were used as simulated patients. Each mannequin is highly technical and motorized; some even react to being touched. The wounds on the mannequins are the same as what would be in a combat zone. Tourniquets, blood transfusions, IV’s and medication training were all a part of the experience—in addition to evacuation, something you wouldn’t find in a regular medical school course.
“Not only are we helping hone emergency medicine skills,” Fisher said, “but also learning in this type of environment and in the context of combat casualty care adds another layer of meaningful and real world applicability they wouldn’t get in a traditional medical school training environment.”
The course was open to all students across the medical school. Fisher hopes to have several more of these training courses throughout the year.
###
This story by Katherine Hancock originally appeared in Vital Record.