What The Delta Variant Means For COVID-19
The highly contagious Delta variant has caused a surge in COVID-19 infections and hospitalizations, largely among the unvaccinated. This latest development in the coronavirus pandemic has renewed debates about masking, vaccines and public health protocols as Americans continue to return to offices and schools.
Texas A&M Today spoke about the current state of the pandemic with Dr. Gerald W. Parker, director of the Pandemic & Biosecurity Policy Program within the Bush School of Government and Public Service and associate dean of Global One Health at the College of Veterinary Medicine & Biomedical Sciences, and Dr. Peter Hotez, dean of the National School of Tropical Medicine at Baylor College of Medicine and co-director of the Center for Vaccine Development at Texas Children’s Hospital. At Texas A&M University, Hotez was a 2019-2020 faculty fellow with the Hagler Institute for Advanced Study and is a senior fellow emeritus at the Scowcroft Institute of International Affairs at the Bush School.
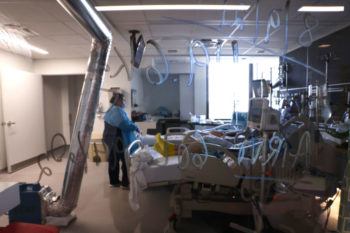
What’s your assessment of where we are at this stage of the pandemic in the United States, given the percentage of the population that is fully vaccinated and the surge in COVID-19 infections?
Parker: The SARS-CoV-2 virus continues to move through the population worldwide, adapting with new variants to favor its own survival and continued transmission to vulnerable individuals.
The good news: the biomedical research enterprise and vaccine industry were able to accelerate the development of safe and effective COVID vaccines – without cutting quality, safety and efficacy corners – in only 11 months after the first genomic sequence of SARS-CoV-2 was published. That was a remarkable public health achievement that was followed by the largest and most complex mass vaccination campaign in public health history. The vaccination campaign was understandably bumpy at first until vaccine production stabilized, healthcare systems vaccinated front-line health care providers at highest risk of exposure, and state and local authorities geared up mass vaccination sites in urban centers and other means to reach underserved communities and rural areas across Texas and the United States. As vaccine coverage increased from January to May, new daily COVID cases, hospitalizations and deaths dropped precipitously from their January 2021 highs.
As of Aug. 9, there are have been 407,560,705 vaccines delivered and 351,933,175 vaccine doses administered. Fifty percent of the United States population is fully vaccinated with over 80 percent of the most vulnerable, 65 years of age and older, fully vaccinated.
The bad news: vaccination uptake slowed significantly from May through July, 50 percent of the United States population remains unvaccinated, and a new highly contagious SARS-CoV-2 variant, Delta, emerged in India last spring spreading globally. Delta became the predominate strain circulating in the United States and Texas during the summer of 2021.
During July, the incidence of daily new cases and hospitalizations coinciding with Delta’s emergence have increased rapidly. COVID hospitalizations and ICU cases in Texas are surging. As of Aug. 9, we are 66 percent (9,546) of the peak 14,218 hospitalized patients that occurred in January 2021. Across the United States, hospitalizations are 43 percent of the January peak.
Hotez: We’ve underachieved terribly in vaccinating the South, especially among younger people. When you look at the difference (in vaccination rates) in the North and the South, among those over the age of 65, it’s not that much different: it’s maybe 80 percent versus 95-99 percent (in the North). Where the bottom falls out is among young people.
We’re looking at maybe 20 to 25 percent of adolescents in many Southern counties who are vaccinated, compared to over 70 percent in Massachusetts and Vermont, and similar although somewhat higher percentages among young adults. So the big vulnerability in the South right now are all the unvaccinated young people. And that’s what we’re seeing – COVID-19 is just ripping through the Southern states, and we’re seeing lots of young people going into the hospital now.

The CDC now advises that people in high-transmission areas wear masks in indoor public spaces, even if they’ve been vaccinated. Why has the Delta variant prompted this change in mask guidance?
Parker: CDC changed their mask guidance because of the evolving nature of SARS-CoV-2 and the rapid spread of the highly contagious Delta variant. New data show there are increasing breakthrough COVID-19 cases in fully vaccinated individuals. Even though breakthrough cases leading to hospitalization or death are rare, new data also show that fully vaccinated individuals who become infected could be contagious and a source of transmission putting immune compromised and unvaccinated people at risk.
Hotez: It has to do with the fact that the amount of virus in the nasal passages and the mouth appear to be higher from Delta compared to previous lineages, and that even if you’re vaccinated and you have some virus-neutralizing antibodies, you could still be asymptomatically shedding virus. But the truth is there’s some new numbers saying even if that’s true, the amount of time you spread the virus may still be very limited, so that you might be shedding viruses for a shorter period of time. But all of this information is still very preliminary and mostly unpublished.
Ultimately, I still think the vast majority of virus transmission is coming from unvaccinated individuals, and that’s why you’re not seeing a big surge in the North. Essentially most, or in some cases almost all, the adolescents and adults are vaccinated, and this has the collateral benefit, whereas with the low vaccination rates among young people in the South, there’s a lot of virus transmission going on.
Under what circumstances would you advise people to wear a mask?
Parker: The CDC guidance advises individuals, unvaccinated and vaccinated, to wear a mask while indoors around other people and where there is high community SARS-CoV-2 transmission. Cases and hospitalizations are surging in many Texas communities. If you live in a community with high transmission, particularly with a surge in hospitalization and ICU cases, I recommend you follow CDC guidance. If you are unvaccinated, you should consider getting vaccinated.
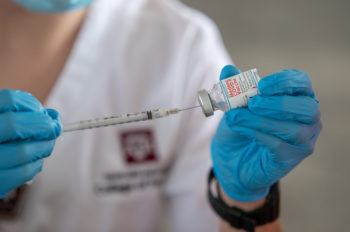
Vaccines are readily available and are by far the most effective tool we have in our toolkit to limit community transmission and reduce the risk of severe disease and death.
Hotez: Clearly, if you’re unvaccinated you should be wearing a mask at all times in indoor settings.
And if you’re vaccinated: I’m still avoiding big indoor crowds, and in which case I’m wearing a mask if I have to be indoors. I don’t go to stores a lot. I’m basically going from work to home most of the time. The only difference now is on the weekends we would take our youngest son and his girlfriend out to dinner and I wouldn’t wear a mask inside the restaurant. Now, with this level of virus transmission, I’m thinking twice about that and starting to go back to DoorDash again.
What do breakthrough infections tell us about the effectiveness of the currently available vaccines?
Parker: To date, the COVID vaccines authorized by the FDA for use in the United States continue to work well, but no vaccine is 100 percent effective. Reports of vaccine breakthrough cases are increasing as new variants emerge and time duration increases from the initial date of completing the vaccination series for many people.
The Phase 3 clinical trial results for Pfizer BioNTech and Moderna vaccines showed 95 percent and 94 percent efficacy against symptomatic COVID-19 illness caused by the original SARS-CoV-2 strains in circulation during the fall of 2020 after two shots. Johnson & Johnson’s vaccine showed 66 percent efficacy against moderate COVID-19 illness and 85 percent efficacy against severe illness after one shot.
The clinical trials did not measure protection against asymptomatic infection or potential to transmit SARS-CoV-2 after vaccination. Nonetheless, the Phase 3 clinical trial results were extraordinary, far exceeded the FDA efficacy threshold of 50 percent, and gave hope that vaccines could control the most severe outcomes of the pandemic.
As of Aug. 9, more than 350 million vaccine doses have been administered and 166 million people were fully vaccinated, 50 percent of the United States population. CDC has received reports of 7,525 hospitalizations or deaths in vaccinated people diagnosed with SARS-CoV-2 infection compared to over 35 million confirmed COVID-19 cases. In about 25 percent of the breakthrough cases, patients were asymptomatic, or their diagnosis appeared secondary to primary cause of hospitalization. This indicates what we knew when the vaccination campaign started and what we know now: vaccine breakthrough cases are expected.
“Vaccines are readily available and are by far the most effective tool we have in our toolkit to limit community transmission and reduce the risk of severe disease and death.”
To date, available data show vaccine breakthrough cases leading to hospitalization or death appear rare and only represent a small percentage of COVID cases. Vaccine breakthroughs are more likely to occur in congregate settings, such as nursing homes, and in populations at risk of vaccine failure (immune compromised, elderly and others).
But CDC’s data has limitations because they are dependent on passive reporting from states on vaccine breakthroughs that led to hospitalization or death and does not include asymptomatic or symptomatic mild to moderate infections.
Population-based studies are needed to gain an understanding of estimated rates of breakthrough cases against mild to moderate infection, vaccine effectiveness against emergency variants, and durability of immunity.
Clinical trials and real-world studies confirm the safety and effectiveness of the Moderna and Pfizer BioNTech COVID vaccines. Through the end of July, the data tells us Pfizer BioNTech and Moderna COVID vaccines remain remarkably effective at reducing risk of hospitalization, severe disease and death for individuals, even for the Delta variant.
Hotez: The vaccines are still really robust. They still give high levels of protection, they’re keeping you out of the hospital and preventing you from symptomatic illness. But there’s increasing information regarding breakthrough cases, and new information in a preprint publication from the Mayo Clinic that protection from non-hospitalized COVID infection may have decreased to the 40-50 percent range for the Pfizer-BioNTech vaccine, with similar data from Israel.
Moreover, when the breakthrough cases happen, they’re associated with higher virus loads. But that’s new information.
We don’t know if this represents true waning immunity versus decreased virus neutralizing antibody against the Delta variant. It’s also important to remember, the way the vaccines were designed was they were tested on their ability to stop symptomatic infection, hospitalization and death, and that mostly still holds. We haven’t lost that, so we should be very mindful that the vaccines still work well.
What challenges are officials seeing with vaccination rates? Are there methods that could be implemented to reach more people?
Parker: Vaccine rates have increased as cases and hospitalizations surge due to Delta, but not enough.
Vaccines are readily available and continue to work remarkably well to reduce risk of hospitalization, severe disease and death. Public health authorities and community leaders should approach the importance of vaccination with more reasoned, calm and reassuring discussions about vaccine safety and effectiveness to gain public confidence in vaccines for those who remain undecided.
The recent change in the CDC mask guidance was prudent and in line with good public health action, but the way the message was delivered caused confusion, controversy and unnecessary arguments, largely because the data underlying the mask guidance change was not made publicly available and discussed in a reasoned approach until several days later. Unfortunately, the ensuing controversy lost focus on the reassuring message about vaccine safety and effectiveness.
I encourage everyone to talk with their health care provider, family physician, or other trusted people in your community to obtain the best information available from trusted sources when trying to reach a decision to get vaccinated.
Data on COVID vaccine safety and effectiveness is reassuring compared to not being vaccinated. SARS-CoV-2 can take a life away in mysterious and sometimes unpredictable ways. COVID vaccines authorized for use in the United States remain remarkably effective against the most severe clinical outcomes from SARS-CoV-2 infection, including Delta. COVID vaccination is the best way to protect yourself, your family, and colleagues.
Finally, I think it essential that the FDA expedite their final review and grant full Biologics License Approvals for the COVID vaccines.
Hotez: I’m quite worried about the schools because there’s so much transmission now in the Southern region, and the vaccination rates among adolescents are really low. Everyone’s talking about mask mandates for schools, but I think we need to move toward vaccination mandates, and that’s going to be really important if we’re going to have a successful school year. Otherwise, we’re already seeing so many kids getting COVID as schools start to open – it’s just going to shut everything down. I think we need to reprioritize getting kids safely through the school year and in-person classes, and that’s going to mean both vaccine and mask mandates. Even though that’s not popular, I don’t see another way around it.
The anti-vaccine aggression is still pretty high. We still need to address the disinformation that still dominates the media and social media.
Has the Delta variant affected the threshold for herd immunity? Is that still the goal?
Parker: Unfortunately, I do not have a good answer for herd immunity, nor do I believe anyone has a good answer beyond predictive modeling or predictive speculation.
I do not believe the SARS-CoV-2 virus is going away anytime soon. We cannot eliminate SARS-CoV-2 by human interventions, but human interventions can reduce the virus’s impact. We should anticipate that the virus will become endemic with new variants emerging beyond Delta. But that does not mean the pandemic will go on forever. The pandemic will not go on forever if we can mitigate the most severe clinical outcomes even if SARS-CoV-2 becomes endemic. Other viruses, like influenza, are endemic and we learn how to manage risk – that includes annual vaccinations.
The current COVID vaccines remain remarkably effective in reducing the risk of severe disease and death, even against the highly contagious Delta variant. More people should take advantage of this life saving measure. The United States and other high-income countries must take more action to increase global vaccine access. The WHO reports that less than 2 percent of people living in low-middle income countries are fully vaccinated.
Finally, Pfizer, Moderna and Johnson & Johnson are conducting new clinical trials with vaccine candidates designed against new variants and are prepared to pivot manufacturing boosters against specific new variants, like we do every year for seasonal influenza. National public health authorities must likewise be prepared to make timely and decisive decisions for the pivot to be effective.
Hotez: I don’t even use the term herd immunity anymore because it’s been so twisted by people with political agendas. What I say is once vaccination coverage gets to about 75 percent among the whole population, we start to see a slowing in transmission, and that’s the goal. Based on the reproductive numbers of this virus, if we’re serious about stopping transmission, ultimately we have to get 85 percent of the population vaccinated. That’s all of the adults and adolescents. It’s a pretty high bar, but I think we could do it.
Media contact: Caitlin Clark, caitlinclark@tamu.edu


