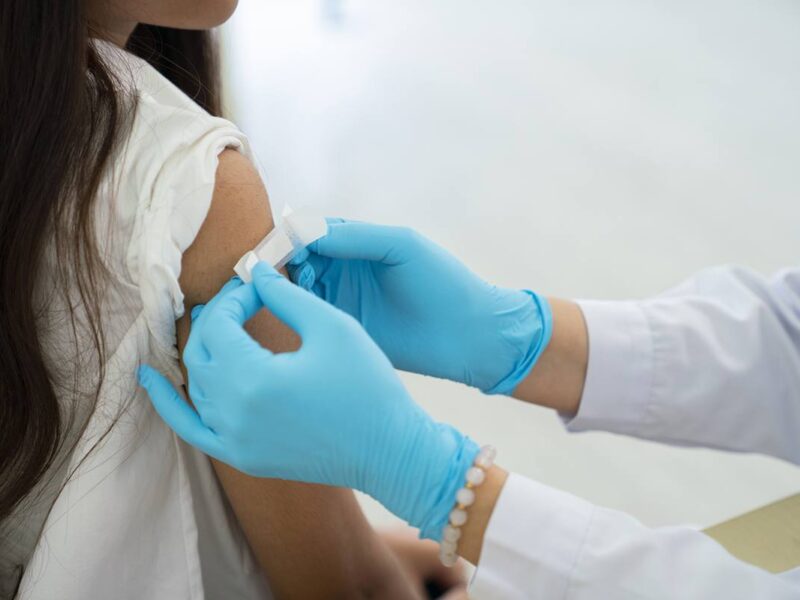
If We Get A Vaccine, What Then?
Researchers around the world, including at Texas A&M University, are working to create a COVID-19 vaccine as global deaths number at more than 390,000. We asked Gerald Parker, associate dean of Texas A&M’s Global One Health, and Timothy Callaghan*, an assistant professor in the School of Public Health, to give us their assessments regarding vaccine development and rollout, as well as the possible effects if people refuse it.
How long before we have a vaccine?
Callaghan: While we are on the path to a vaccine for COVID-19, we need to recognize that the development and distribution of a vaccine will not happen anytime soon. Americans need to be prepared to continue social distancing, washing their hands, regularly wearing masks, and following all recommended guidance well into 2021. By doing that, we can keep as many Americans as possible safe and healthy until a possible vaccine arrives in the next 12-24 months.
Parker: Assuming we successfully develop a safe and effective vaccine, the most optimistic projections report that we should have a vaccine in 12-18 months. I believe it will take at least 24 months. It will take time to build up the supply chain and distribution channels to enable wide public use in the United States. Initial vaccine supplies will be limited. Front line health care providers, emergency responders, and high-risk individuals will be the first cohorts to receive the vaccine until supplies build up. We must also consider how to provide access to this scarce medical resource to low-middle income countries.
Can the vaccine be mandated?
Callaghan: It could be quite difficult from a political perspective to mandate that all Americans get vaccinated against COVID-19. That said, based on the Supreme Court’s ruling in Jacobson v. Massachusetts in the early 1900s, we know that constitutionally, the government has wide latitude to protect the public’s health. In that case, the Supreme Court upheld the legality of fining a Massachusetts pastor for refusing to vaccinate against smallpox. Interestingly, the court ruled that fining individuals for non-compliance was constitutional but that the state could not forcibly vaccinate anyone. In the context of COVID-19, this would suggest that states or the federal government could mandate vaccination and punish non-compliance with fines, but they could not actually force anyone to vaccinate.
Will the COVID-19 vaccine be on the list of shots for school children, like measles, mumps and rubella?
Parker: We are several years from having to address vaccine recommendations for children. Fortunately for now, children are not at high risk of serious COVID-19 disease and death, but we continue to learn more about COVID-19 and that could change. However, children are likely asymptomatic carriers, thus a vaccine may be important to help build and maintain herd immunity, as well as to protect children from becoming symptomatic once a vaccine is available for children. At that time, public health authorities and school districts will make evidenced-based decisions regarding COVID vaccine requirements for school-aged children guided by public health and medical recommendations.
Based on current trends in anti-vaxxing, how many people do you think will refuse to be vaccinated?
Callaghan: We know that vaccine hesitancy is widespread in the general public, but that the percentage of Americans who actually refuse recommended vaccines is generally low and varies by vaccine. Assuming a safe vaccine can be developed and affordably administered, most Americans will pursue getting vaccinated. Early opinion polling however suggests that almost a quarter of Americans would be unwilling to be vaccinated against COVID-19 if a vaccine were to become available. Interestingly, polling also suggests that some Americans might eventually vaccinate, but are hesitant to do so right away and might wait until others have already vaccinated and demonstrated its safety.
What will be the effects if people refuse the vaccine?
Callaghan: Beating the coronavirus will require us to reach the point of herd immunity, which dramatically reduces the ability of the virus to spread. This can only happen through two mechanisms – either large numbers of Americans need to get vaccinated against COVID-19 or they need to get COVID-19. As rates of non-compliance to vaccination go up, it sadly means that more individuals will be infected with COVID-19 on the road to herd immunity. This likely means that more Americans will get ill and die from the virus.
Do you have any final thoughts?
Parker: It is likely that the SARS-CoV-2 virus will be with us for some time. We are close to flattening the curve. Immunization will be an important tool in our response tool kit. However, it will not be the only tool. Now we should manage the curve to mitigate dangerous resurgence of disease and a potential second wave in the fall through continued social mitigation measures, personal infection control hygiene, as well as testing, contact tracing, and isolation to box the virus in. We will beat this virus.
* This link is no longer active and has been removed.
Media contact: Lesley Henton, lshenton@tamu.edu