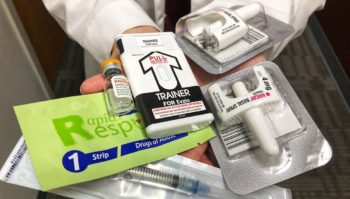
Training To Reverse Opioid Overdoses
With more than 130 Americans dying each day from opioid overdose, the Texas A&M University Health Science Center is responding, advancing training and education in pain management and substance abuse in innovative ways. Texas A&M is the first health science center in the nation to commit to train every health professions student to administer a reversal agent to opioid overdose victims, and save lives.
Through the intensive 90-minute Opioid Overdose Education and Naloxone Administration (OENA) program, the institution will train every Texas A&M Health Science Center student across the state—totaling more than 5,000 students from the colleges of dentistry, medicine, nursing, pharmacy and public health—to recognize an opioid overdose and administer naloxone, a drug that can be administered as a nasal spray or injection to reverse the deadly effects of opioid overdoses.
The reversal agent is available as prescription medication, and some states, including Texas, allow naloxone to be distributed by pharmacists to the public without a prescription from a physician via a standing order. Texas also passed legislation allowing for community distribution of naloxone rescue kits by trained individuals to the general public in response to the rising crisis. Anyone is allowed to possess naloxone without a prescription, and use it in good faith to save the life of a person believed to be suffering from an opioid overdose.
“Naloxone is a life-saving treatment to help until emergency personnel arrive,” said Joy Alonzo, M. Engineering, PharmD, clinical assistant professor at the Texas A&M College of Pharmacy, who is leading the naloxone training effort at the Health Science Center. “The goal is to train our students how to administer naloxone and also educate them about the health care needs of the opioid crisis and spread that awareness to others.”
Alonzo is a member of the institution’s Opioid Task Force, which was formed in 2018 to reduce burdens from the opioid epidemic through collaborative action in research, education and community outreach, across the health sciences. Training of all health professions students is an important component of both the education and community outreach initiatives of the task force.
“Whenever you’re faced with a crisis, you need creative solutions,” said Carrie L. Byington, MD, vice chancellor for health services at The Texas A&M University System, senior vice president of the Texas A&M Health Science Center and dean of the Texas A&M College of Medicine. “The best ideas come when multiple viewpoints are at the table, and that’s the idea behind our interprofessional Opioid Task Force. Together, we’re reducing the stigma associated with opioids, and empowering the next generation of health care professionals to become advocates for naloxone administration within their own communities, wherever they may practice after graduation.”
Students are already putting what they’ve learned to practice. Pharmacy students, who were trained early on through Operation Naloxone, are now actively training first responders and members of the community in how to recognize an overdose and administer naloxone.
“We have seen five reversals from trainings provided to communities,” Alonzo said. “We’re preventing overdose deaths in our communities, and providing opportunities for people with opioid use disorder to access treatment and recovery—saving lives.”
The task force’s efforts also translate well beyond Texas’ borders. Task Force representatives, including Byington and Alonzo, are engaged at the national level, with the American Medical Association Alliance and the Association of American Medical Colleges.
There’s also an evaluation component planned. “We’re going to survey the students on the effectiveness of the training, and then we’re going to re-survey them every 12 months until they graduate to see what sticks and how their attitudes about opioid use disorder changes,” Alonzo said. “We need to change the perspective of the next generation of health care providers, and this initiative is one component of that.”
The ultimate goal is to destigmatize substance use disorders and teach providers—and society in general—to consider it a chronic health condition, not a lack of willpower or a character flaw. Naloxone doesn’t solve the problem or help people overcome addiction, but it does save their lives so they have the opportunity to seek treatment.
“This sort of training should be very common, just like people are trained in CPR,” Alonzo said. “You may never need it, but if the situation does arise, you need to know how to do it right and feel confident that you can save a life.”
This article by Christina Sumners originally appeared in Vital Record.